Results from Study 309/KEYNOTE-775
Vicky Makker, MD, presents the results from Study 309/KEYNOTE-775, as well as key safety findings.
Episodes in this series

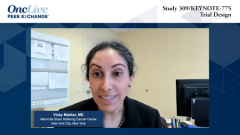
Vicky Makker, MD: We had 827 patients who were randomized between the 2 arms, and the arms were very well balanced with regard to patient age, prior RT [radiotherapy] ECOG performance status, and race distribution. Approximately 85% of patients in both arms were pMMR [proficient mismatch repair]. Most of the patients were White, and approximately 21% were Asian. The full histologic spectrum was on display. The most common subtype, as expected, were patients with endometrioid adenocarcinomas, and they represented approximately 60% of cases in both arms. Serous histology was the most common nonendometrioid subtype, at 25%, followed by clear-cell mixed histologic subtypes. Their proportions are relatively balanced.
In this study, 79% of patients in the lenvatinib-pembrolizumab arm and 76% in the TPC [treatment of physician choice] arm had 1 prior platinum therapy, which means approximately 80% of patients had not received platinum rechallenge prior to lenvatinib-pembrolizumab therapy. And 55% in the lenvatinib-pembrolizumab vs 60% of patients in the TPC arm had prior neoadjuvant or adjuvant treatment.
With regard to the median PFS [progression-free survival] for the pMMR cohort and all comers, what we saw was that there was an early separation of the Kaplan-Meier curves, in favor of the lenvatinib-pembrolizumab activity. It was observed around the first radiologic assessment. The median PFS for the pMMR cohort was 6.6 months vs 3.8 months for lenvatinib-pembrolizumab vs TPC, and as we all saw, the hazard ratio was 0.6. In all comers, the median PFS was 7.2 months vs 3.8 months for lenvatinib-pembrolizumab vs TPC. The hazard ratio was 0.56. What we learned is that PFS was significantly longer with lenvatinib-pembrolizumab vs TPC regardless of the MMR status. Lenvatinib-pembrolizumab also demonstrated a PFS, and for that matter, an OS [overall survival] benefit in all subgroups that were analyzed, including MMR [mismatch repair] status, histology, and prior lines of therapy in all-comer participants vs TPC.
With regard to OS, approximately 9% of patients had informal crossover because lenvatinib-pembrolizumab was approved in many countries at the time that this study was ongoing. Despite that, with a median follow-up of 11.4 months, lenvatinib-pembrolizumab significantly prolonged overall survival in pMMR and all-comer participants. The median OS for the pMMR cohort was 17.4 months vs 12 months for lenvatinib-pembrolizumab vs TPC. The hazard ratio was 0.68. Median OS for all comers was 18.3 months vs 11.4 months for lenvatinib-pembrolizumab vs TPC. The hazard ratio was 0.62. As we saw for PFS, the capital markers were clearly separated at approximately 3 months in favor of lenvatinib-pembrolizumab.
With regard to the objective response rate, it was at least doubled with lenvatinib-pembrolizumab vs TPC in pMMR and all-comer participants. In the pMMR cohort, it was 30% vs 15%, and in all comers it was 32% vs 15% in favor of lenvatinib-pembrolizumab. CR [complete response] and PR [partial response] rates were also approximately double for lenvatinib-pembrolizumab, and more patients in the treatment of physician’s choice group had a better response of progressive disease compared with lenvatinib-pembrolizumab by about 2-fold. It is also important to note that the responses were rapid and durable in both the pMMR and all-comer cohorts with the combination.
Median time to response and the pMMR cohort was 2.1 months vs 3.5 months for lenvatinib-pembrolizumab vs TPC. For all-comers, the response time was 2.1 months for both arms. As far as the median duration of response is concerned, in the pMMR cohort, it was 9.2 months vs 5.7 months for lenvatinib-pembrolizumab vs TPC. For all comers, it was 14.4 months vs 5.7 months, which is in favor of lenvatinib and pembrolizumab.
With regard to treatment exposure and safety discontinuation, which is an area that we’re all very concerned about and focused on, as we of course should be, it’s important to keep in mind that the median duration on treatment was more than double for the lenvatinib-pembrolizumab arm at 231 days vs 105 days for TPC. This could certainly account for the difference in the rate of TEAEs [treatment-emergent adverse events] that were seen between the 2 arms. Nonetheless, grade 3 or greater treatment-emergent adverse events occurred in 89% vs 73% of patients on lenvatinib-pembrolizumab vs treatment of physician’s choice. Lenvatinib dose reductions occurred in 67% vs 13% of patients on TPC. Interruption occurred in 69% of patients on lenvatinib-pembrolizumab vs 27% on TPC. Lenvatinib was interrupted in 59% pembrolizumab and 50%, and both were interred in 31%. Discontinuation rates were 33% on lenvatinib-pembrolizumab vs 8% on TPC. Lenvatinib was discontinued at 31%, pembrolizumab in 19%, and both in 14%, which we can talk more about. I’m sure we will.
As expected, the safety profiles of lenvatinib-pembrolizumab and TPC are different. That was not surprising. Overall, the safety profile of lenvatinib-pembrolizumab was generally consistent with both of the individual agents. The most common any-grade TEAEs on lenvatinib-pembrolizumab, not surprisingly, were hypertension and hypothyroidism, which was predominantly grade 1 or grade 2 and was easy to manage. These also included diarrhea, nausea, and decreased appetite. With the TPC, it was anemia, nausea, neutropenia, and alopecia. Lenvatinib-pembrolizumab, as I said, had more grade 3 to grade 5 TEAEs. They occurred in 89% of patients, and the most common were hypertension in 38%, followed by weight decrease, decreased appetite, and diarrhea. Each of these, though, occurred in 10% of patients or fewer. Grade 3 or greater events occurred in 73% of patients in a TPC. As we would expect, there were cytopenias. Regardless of causality, grade 5 events occurred in 5.7% of patients on lenvatinib-pembrolizumab vs 4.9% of patients on TPC. Those are the bulk of the data, so I’ll stop there.
Brad Monk, MD, FACOG, FACS: That’s so much, and it’s a lot to digest. You have to hear it a couple of times. Did you just tell us that the overall survival benefit at the median was greater than PFS? Is that what you said?
Vicky Makker, MD: The overall survival for the pMMR cohort was 17.4 months vs 12 months. With regard to PFS, the PFS for the pMMR cohort was 6.6 months vs 3.8 months. That’s right.
Brad Monk, MD, FACOG, FACS: There is a 5-month overall survival but only 3 months of PFS. Did that surprise you? Generally, overall survival is lower than PFS. In fact, we’ll frequently do PFS and no overall survival. This is reversed. This is a greater overall survival advantage than what you did for PFS. Did that surprise you?
Vicky Makker, MD: It did, but this is not a pattern that’s so unusual for immuno-oncology drugs, so this wasn’t so unexpected. Frankly, for me, it was encouraging to see this because it is the gold standard. Overall, I was very encouraged by the data.
Transcript Edited for Clarity