Insight on Ongoing Trials in EC
Key opinion leaders take a look at the evolving treatment landscape in endometrial cancer, discussing ongoing trials in the space.
Episodes in this series

Brad Monk, MD, FACOG, FACS: Let’s transition to discuss patients with recurrent endometrial cancer, or stage IV. They have the same risk of recurrence and death. Vicky, you’re a passionate advocate of this pembrolizumab-lenvatinib combination. You presented these data, which we’re very excited about. But we now have a study on the front line, right?
Vicky Makker, MD: That’s right.
Brad Monk, MD, FACOG, FACS: It’s a chemotherapy-free regimen vs carboplatin-paclitaxel. Tell us about that.
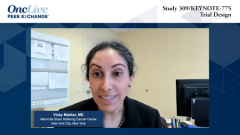
Vicky Makker, MD: Sure. This is based on the promising phase 2 results, and now the results of Study 309/KEYNOTE-775. This is essentially a randomized open-label trial to compare the safety and efficacy of lenvatinib plus pembrolizumab in combination vs carboplatin-paclitaxel chemotherapy as first-line treatment for patients with advanced or recurrent endometrial cancers. Essentially, patients who have stage III or stage IV recurrent endometrial cancer will be eligible. They may have received chemotherapy only if it was administered concurrently with radiation therapy, and patients will be randomized 1:1 to lenvatinib at 20 mg orally once daily, plus pembrolizumab at 200 mg every 3 weeks vs the standard paclitaxel-carboplatin IV [intravenous] every 3 weeks. The study has a dual primary end point of PFS [progression-free survival] and OS [overall survival]. The study is close to accrual, so we’re really happy to see that it accrued, and we’re looking forward to the data.
Brad Monk, MD, FACOG, FACS: I was a little skeptical until I saw the results of Study 309/KEYNOTE-775. Whoa—this whole idea of a chemotherapy-free regimen, which is what the study is, is so exciting. I’m excited, and I’m glad that it did enroll. Let’s continue this conversation. There are 3 ways to make anti–PD-1 and anti–PDL-1 agents better. One is to add a VEGF, and you told us about adding lenvatinib. The second is to add chemotherapy and radiation, and that’s what we’re going to talk about next. Certainly, the third would be an additional checkpoint inhibitor such as an anti-TIGIT or a CTLA4. But let’s talk about this idea of adding chemotherapy to checkpoints. This is the second opportunity to make single-agent checkpoints better. Nicoletta, 3 studies try to answer that question of I/O [immuno-oncology] therapy vs chemotherapy in the recurrent metastatic setting. Talk to us about those 3 studies.
Nicoletta Colombo, MD, PhD: You’re right. There are 3 trials that include more or less the same populations. We are talking about recurrent or metastatic advanced endometrial cancer, with all comers in all trials. They are stratified according to their MSI [microsatellite instability] status, but all comers are included. The first trial is the NRG-GY018 study, and it’s looking at a combination of carboplatin and paclitaxel plus a pembrolizumab placebo in treating stage III or IV recurrent endometrial cancer. pembrolizumab is the I/O together with carboplatin-paclitaxel. The other trial is the RUBY trial, and that accepted the same design, but dostarlimab is used instead of pembrolizumab plus chemotherapy or a placebo. It’s a study of the same population with the same stratification factors. The AtTEnd study is again, the same design, but it uses atezolizumab. We have patients with advanced or recurrent endometrial cancer. It’s a phase 3 placebo-controlled study enrolling patients. As far as I know, the first part of the RUBY trial is completed. Now it’s open for a second phase, which is a little different in the design. AtTEnd is also enrolling. We enrolled more than 350 patients, so we hope to conclude the accrual by the end of the year. I don’t have the details on the accrual, but I think it’s still enrolling patients. These are the 3 very similar trials; the statistical design is a little different, but they all look at OS and PFS. In the RUBY trial the primary end point is PFS, but they will look also at OS. In the AtTEnd trial, we have OS and MRD [minimal residual disease] as the primary end point. These are the 3 ongoing trials in the front line.
Brad Monk, MD, FACOG, FACS: NRG-GY018 uses pembrolizumab, RUBY uses dostarlimab, and AtTEnd uses atezolizumab. In the NCI [National Cancer Institute]–funded GY018, the MSI-high cohort is separate. It’s completely powered and completely analytical rather than welcoming all comers. It’s 2 studies rolled in 1, but you’re right. They’re very similar. Dave, what do you think of PARP inhibitors in treating endometrial cancer? You mentioned that RUBY will include that, but we do have a trial with durvalumab. Dave, tell us about DUO-E and how that’s different.
David O’Malley, MD: The DUO-E trial is also looking at a carboplatin-paclitaxel backbone with durvalumab followed by durvalumab maintenance plus or minus olaparib. We’re really looking at this subpopulation of patients who are potentially going to benefit. We have talked about serous cancer, with the uterus being more similar to what we see in ovarian cancer—not molecularly; that is somewhat true—but there are some significant differences when we look at them molecularly. For me, it does make sense that some of those patients with TP53 mutations are going to benefit.
Brad Monk, MD, FACOG, FACS: Kara, you had mentioned the RAINBOW trial. Now we have, I guess, RUBY part 2 or DUO-E— RAINBOW with PARP inhibitors. It seems as if we might really answer this important question. What do you think about PARP inhibitors in treating endometrial cancer?
Domenica Lorusso, MD, PhD: They may play a greater role, particularly for patients with TP53 mutations. For sure, we will see the results of this trial, and then we will better define when to use it in the algorithm of treatment, if we should use it in the adjuvant setting or in the first-line metastatic setting. Then we’ll see the results in treating ovarian cancer or how we can use PARP, which is another possible strategy, but they’ll play a role alone or in combination with immunotherapy.
Brad Monk, MD, FACOG, FACS: It’s been fun to develop this collaboration between ENGOT [European Network of Gynaecological Oncological Trial groups]—which is your group, Dave—and my group, GOG [Gynecologic Oncology Group]. With that collaboration, we can do all these trials. Many people would say they compete. We started our conversation—it’s good to have lots of opportunities in the trials, are different in subtle ways. I’m excited, and I’m grateful and thankful for that collaboration. There’s a whole other class of agents. There’s this trial called ENGOT-EN5, or SIENDO. Vicky, I know you’re pushing the envelope with these novel agents. Tell us about that study.
Vicky Makker, MD: This trial is evaluating an agent called selinexor, which is a novel oral selective inhibitor of nuclear export. Essentially, this agent forces the nuclear retention and activation of tumor-suppressor proteins. This drug, in combination with low-dose dexamethasone, is already approved to treat relapsed/refractory multiple myeloma. It’s also approved to treat relapsed/refractory diffuse large B-cell lymphoma. It has shown activity across a number of other hematologic malignancies and solid tumors. It has shown some efficacy treating endometrial cancers that have been previously treated. In the absence, as yet, of an approved maintenance therapy for patients with endometrial cancer following a platinum-based therapy, this drug is being evaluated in a maintenance setting in patients who have achieved CR [complete remission] or PR [partial remission] following platinum and taxane chemotherapy.
Brad Monk, MD, FACOG, FACS: This study is interesting based on its mechanism of action, which you talked about, and also the setting. This is the Athena of endometrial cancer: You finish your chemotherapy, and then you’re randomized. All options need to be on the table. All classes of agents need to be studied. It’s collaborative, as that trial is, the ENGOT-GOG collaboration.
Vicky Makker, MD: Absolutely.
TRANSCRIPT EDITED FOR CLARITY